Macular Disease
Macular disease is any disease or degeneration of cells in the macula - the center of the retina which is responsible for our straight ahead and sharp, detailed vision.
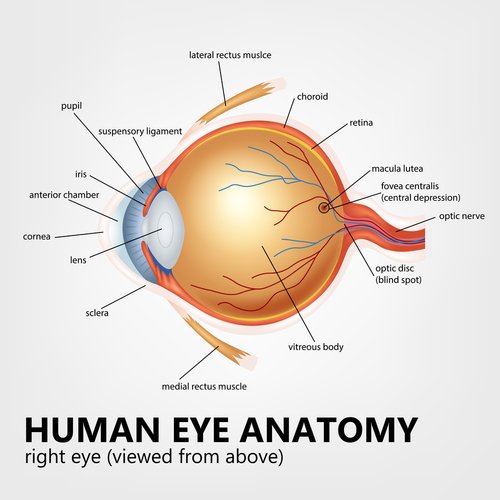
The macula is responsible for our straight ahead or central vision, such as seeing the face of a person or reading a book. Macular eye disease results in a gradual loss of sharp, detailed and central vision. Usually the side or peripheral vision is not affected.
From this macular degeneration picture you can see the macula is a tiny spot in the center of the retina. It is made up mostly of cone cells . They are photoreceptor cells that help transmit images to our brain.
Symptoms can range from mild loss of vision to severe vision loss. They can include:
loss of central vision
blurry vision
loss of night vision
difficulty reading
distorted vision
loss of contrast sensitivity
trouble discerning colors
photophobia or a dislike of bright lights
Definition of Macular Degeneration
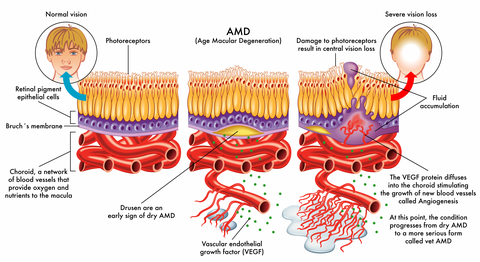
Macular degeneration is a silent and painless loss of central vision due to the degeneration or dying of cells in the retina, called the macula. Macular degeneration or ARMD (age-related macular degeneration), is the leading cause of vision loss in Americans aged 65 and older.
As we age, the supporting tissue to the macula are not functioning as well and do not get the needed nutrients and oxygen to these cells. The transport of these nutrients are affected as well as the removal of waste products.
First, it is important to realize that what is lost is the central portion of your sight - what you see right in front of you like the face of a person or the words in a book. Peripheral or side vision is still there. There are two forms of ARMD:
Dry Macular Degeneration - the most common form; 85-90 percent of AMD patients are diagnosed with dry AMD
Wet Macular Degeneration - only 10-15% of patients are diagnosed with this form that causes a more severe and sudden vision loss
Click here to learn more:
Macular Degeneration Definition
Juvenile Macular Degeneration
Juvenile macular degeneration is a genetic form of macular
degeneration that develops in childhood, teenage or young adult years.
It is usually inherited and causes progressive loss of vision that distorts or blurs what we see straight ahead. This hereditary eye disease forms in both eyes with similar changes in both eyes as well. Macular degenerative disease develops in older people and is called age-related macular degeneration (AMD) while forms of JMD develop in childhood or teen years.
However, many of these inherited retinal diseases have some of the same characteristics as age related macular degeneration.
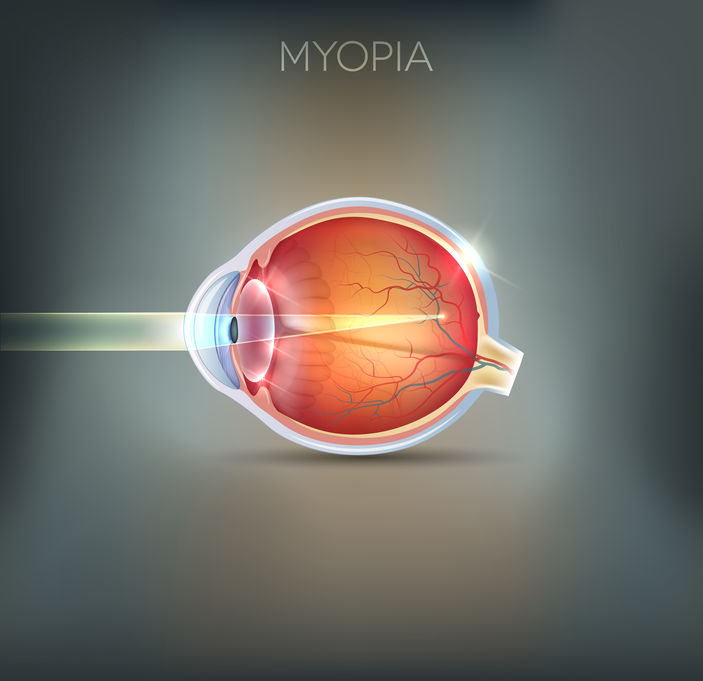
Myopic Macular Degeneration
Did you know that myopia (nearsightedness) puts a person at risk for developing macular degeneration? The longer shaped eyeball can result in the thinning of the retina.
Many adults are surprised by a diagnosis of macular degeneration
in their 30's and 40's assuming that this macular disease occurs mostly
in the elderly population.
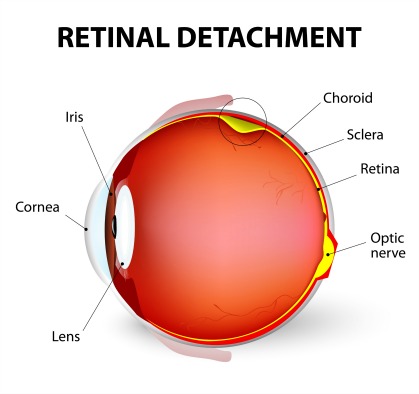
Retinal Detachment
Just like everyone should be aware of the symptoms of a stroke or heart attack, awareness of the symptoms of a detached retina can save your sight or the sight of someone else.
Unlike my uncle who experienced one of these symptoms and because
of the delay in seeing his ophthalmologist he lost his vision in his
right eye.
Find out the top 5 signs of a detached retina here:
Macular Edema
Macular edema is a macular condition that results from the swelling or collection of fluid underneath the macula, the center of the retina. This tiny portion of the retina is responsible for our central, straight ahead and detailed vision. The fluid comes from leaking retinal blood vessels.
Some of the causes are:
1) Diabetes
2) Uveitis
3) Blockage in the small retinal veins or arteries
4) Wet Macular Degeneration
5) Cataract Surgery
6) Repair of a detached retina
7) Eye Injury
8) Side effect of medication
Find out what happens to one's vision when fluid builds up under the macula: Macular Edema
Macular Pucker
A macular pucker is scar tissue that has formed on the macula, which is the center of the retina in the back of the eye.
To learn more about causes, symptoms and treatment.
Macular Hole
A macular hole is a small break in the macula. The macula is a tiny area in the back of the eye in the center of the retina.
It is made up mostly of cone cells.
These photoreceptor cells provide us with the sharp, central vision we need for reading, driving, and seeing fine detail.
These tears are usually related to aging and occur in people over age 60.
Macular Hole Symptoms
Although the symptoms are similar, macular holes and macular degeneration are two separate and different conditions. Symptoms often begin gradually. In the early stage, people may notice
A slight distortion or
Blurriness in their straight-ahead vision
Straight lines look bent or wavy
Reading and performing other routine tasks with the affected eye become difficult.
How It Happens
Most of the eye's interior is filled with vitreous, a gel-like substance that fills about 80 percent of the eye and helps it maintain a round shape.
The vitreous contains millions of fine fibers that are attached to the surface of the retina. As we age, the vitreous slowly shrinks and pulls away from the retinal surface. Natural fluids fill the area where the vitreous has contracted. This is normal.
In most cases, there are no adverse effects. Some patients may experience a small increase in floaters , which are little "cobwebs" or specks that seem to float about in your field of vision.
However, if the vitreous is firmly attached to the retina when it pulls away, it can tear the retina and create a hole.
Also, once the vitreous has pulled away from the surface of the retina, some of the fibers can remain on the retinal surface and can contract. This increased tension on the retina can lead to a macular hole.
In either case, the fluid that has replaced the shrunken vitreous can then seep through that hole which then alters the surface of the macula and causes the distortion in vision.
Three Stages
* Foveal detachments (Stage I). Without treatment, about half of Stage I macular holes will progress.
* Partial-thickness holes (Stage II). Without treatment, about 70 percent of Stage II macular holes will progress.
* Full-thickness holes (Stage III).
The size of the hole and its location on the retina determine how much it will affect a person's vision. When a Stage III hole develops, most central and detailed vision can be lost. If left untreated, a macula hole can lead to a detached retina, a sight-threatening condition that should receive immediate medical attention.
Surgery
Sometimes a macula hole can seal itself and requires no treatment. However, surgery is necessary in many cases to help improve vision. In this surgical procedure-- called a vitrectomy -the vitreous gel is removed to prevent it from pulling on the retina and replaced with a bubble containing a mixture of air and gas.
The bubble acts as an internal, shor term bandage that holds the edge of the hole in place as it heals. Surgery is performed under local anesthesia and often on an out-patient basis.
Following surgery, patients must remain in a face-down position, normally for a day or two but sometimes for as long as two-to-three weeks. This position allows the bubble to press against the macula and be gradually reabsorbed by the eye, sealing the hole. As the bubble is reabsorbed, the vitreous cavity refills with natural eye fluids.
Diabetic Retinopathy
Diabetic retinopathy has many of the same symptoms of macular degeneration. It is a retinal condition that frequently develops in the eyes of those who have diabetes.

Diabetes affects the vascular and circulatory system - of not
just the heart, but other parts of the body as well, including the eyes.
There are many eye conditions or types of macular disease that cannot be corrected by glasses, surgery or other types of treatment. There is some usable vision but it is limited - this is what low vision means.
The key to living with limited vision is to maximize the vision one does have. This can be done with different low vision aids and by training that is offered by low vision specialists.
Go from Macular Disease to WebRN Macular Degeneration Home
√ Prevention of Macular Degeneration?
√ Tips for Daily Living?
√ Food Suggestions for a Macular Degeneration Diet?
√ Ideas on Visual Aids to Maximize your Sight?
If you said "yes" to any of the above, sign up for the monthly Macular Degeneration News.